November 2021
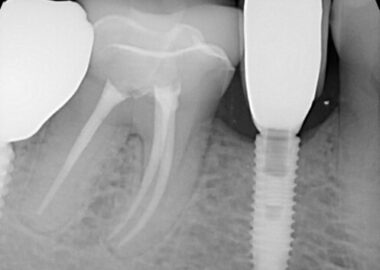
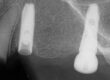
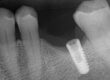
The patient presented on referral from Dr. Z. for retrieval of a fractured abutment screw fragment from a DIO 3.0 implant in the #29 site. By history from the patient, the implant restorative was in for approximately 6 weeks when the screw fractured. Evidently, he had returned to the office with a tight contact issue, but the timing is unclear. When he returned with the loose crown the fractured abutment screw was discovered and he was referred here. There were no previous attempts made at recovery. After discussing the treatment protocols for recovering screw fragments, the area was infiltrated, and a conservative exposure of the implant top was made taking care to spare the thin attached tissue on the facial side. Under the clinical microscope at 25x, the screw fragment was found to be mobile but located just below the implant first thread. This is a Type III case in my treatment algorithm. The fragment was carefully rotated clear of the implant threads and retrieved. The implant was cleaned and in the absence of an appropriate healing abutment a small drop of silicone impression material was placed to act as a temporary healing abutment until the appropriate healing abutment could be installed by his restorative dentist, Dr. Z. The implant was totally intact and the prognosis for the site is unchanged secondary to the screw fracture or the recovery.
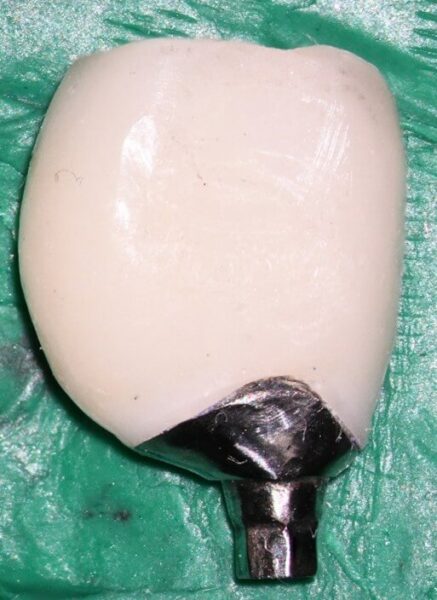
The photo of the recovered crown maybe important as to why this failure occurred so quickly. It appears the crown was finished on the outside diameter of the implant instead of the inner diameter of the 11-degree conus connection. This would have created a vertical stop preventing the total seating of the conus and the friction fit and stability it should provide. I would like to understand how this crown was constructed to see if this theory is, in fact, correct.
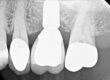
This narrative is an addendum to the original narrative. The assumption is made the reader has already read the original narrative and or has access to it. The last paragraph of the original narrative attempted to reveal a reason for this very early mechanical failure. Due to a lip seen on the supplied photo of the crown, it was postulated a possible reason for failure could have been a vertical interference which would prevent the conus from seating and therefore the abutment to implant connection would not function as designed. Now with examination of the original crown, additional information is presented below shedding more light on the issue. Without a doubt, the lip seen on the original photo had nothing to do with the early failure as this lip is well above the implant abutment junction as seen in the photo below so the postulated interference would not have been present.
So, with that issue resolved are there other reasons for this early failure? I can name four, two of which are probable and possibly worked in unison. The second two I don’t think would have been involved in such an early failure. Let’s investigate the first two.
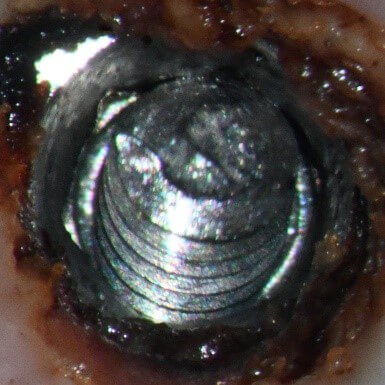
The following photos show two views of the abutment interface along with a photo of a new DIO 3.0 temporary abutment. Please note the worn look of the abutment interface and the crisp machining of the temporary abutment.
The difference here is remarkable when viewed under the microscope. This wear was not caused by the short time in the mouth but rather by lack of interface protection during crown construction, finishing and polishing. To appreciate this to another level, I have placed indicator on the interfaces and reseated both on the new replica. The following photos show how these two surfaces are witnessing.
Note the lack of conus indicating on the left two images as compared to a clearly indicating conus in the image of the temporary abutment on the right. Photographing the abutment was difficult as there was very little rubbing off of the indicator allowing for the underlying shiny metal to indicate the points of contact. Conical connections are friction fit joints and to generate stability rely on length, width, and angle of the conus along with the precision fit of the two mating surfaces. The wear on this abutment shows a lack of attention to detail in the fabrication of the restoration.
Secondly, if my history is correct, the patient had returned for contact adjustment (s) prior to the screw fracture. Combining the abutment misfit, coupled with the possibility of contact issues interfering with the full seating of the abutment connection, I can understand why there was not even short-term stability to this abutment implant connection. It simply was not set up to function as the engineers had designed.
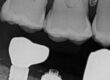
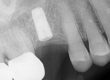
The third reason for failure mentioned above relates to the size of the implant and connection in general. This is a 3.0mm implant which is a copy of the Astra Tech 3.0 Tx implant in all of the critical design features and dimensions. Astra has an FDA clearance for their implant to be used in maxillary laterals and mandibular incisors only. I don’t know if the same holds true for this DIO copy, but I would assume so. Why is this an issue in a small diameter implant? A 3.0 two-piece implant can only be made to withstand a certain amount of force. A posterior application will generate significantly greater force on the implant pillar than in an anterior application, hence the FDA ruling. This additional load stresses the connection and the force will be magnified more by torsional loading (force x leverage arm). In the following photograph it can be seen the restoration has a buccal cantilever due to lingual implant position.
This crown is narrow in the mesial to distal direction which limits torsional loading on that axis but in the buccal lingual direction there will be torsional loading to the buccal. However, I don’t believe these two factors would have been the cause of failure, as this happened so fast. The limited number load cycles would not have had time to produce the necessary fatigue. If this would have happened a few years from now, then it would definitely be a consideration along with any bruxing or diet habits which would have compounded the loading on the narrow diameter implant.
I hope this helps clarify the mechanics, physics, and probably mostly, lack of detail in construction and delivery.